The quality of primary care in the UK is declining and inequality is on the rise. In England alone, treating illness arising as a result of these inequalities cost the NHS £5.5 billion each year [Marmot review,2010]. It is noteworthy that while healthcare inequality impacts people from all walks of life, ethnic South Asians, who make up nearly 4.43 million people, have a much worse health-related quality of life compared with their white British counterparts [Census-2021, Sutton.M, Lancet, Jan-2021].
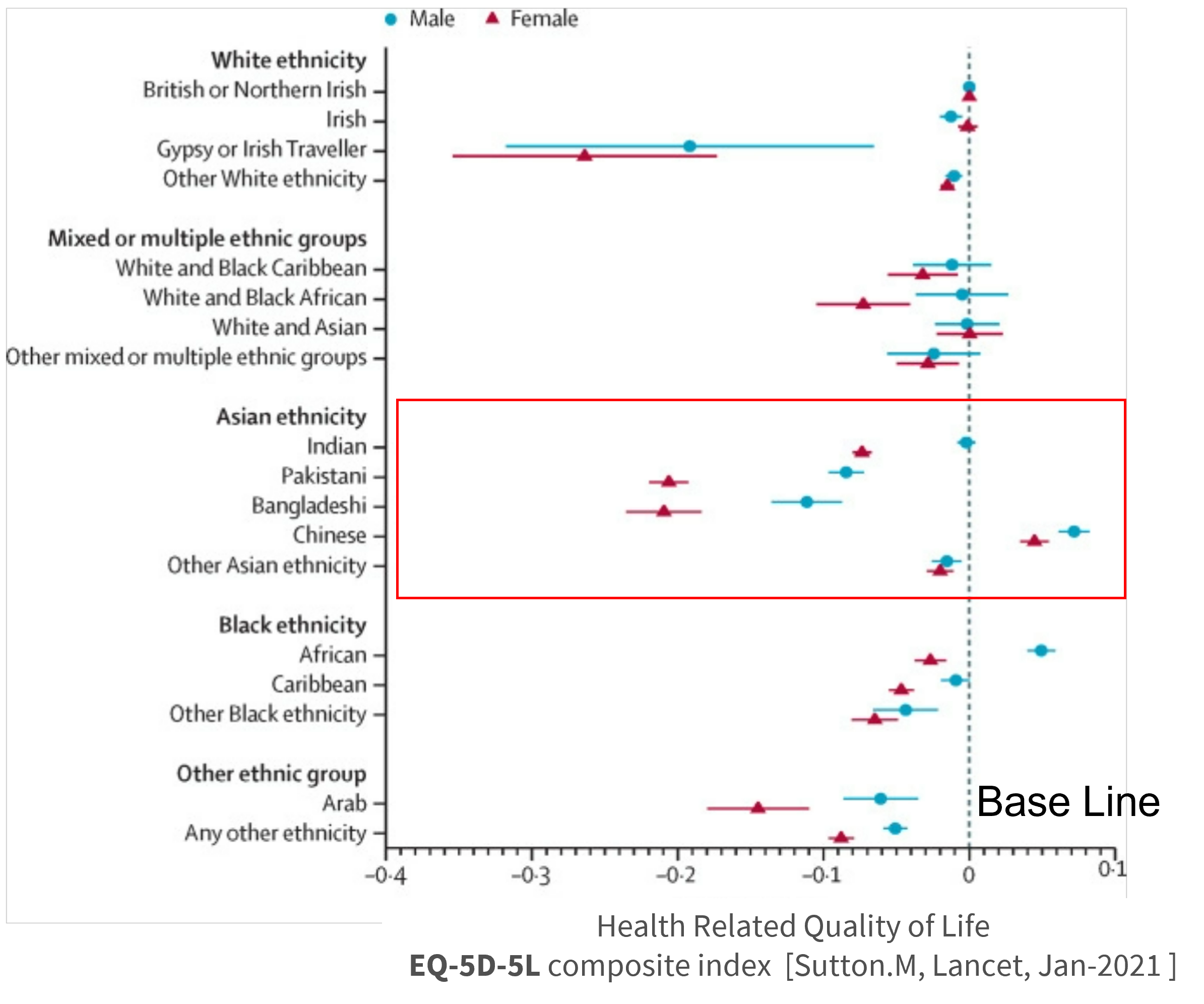
For many south Asian patients language and cultural barriers are the two biggest challenges when establishing the first communication with the primary care system. Approximately 30% of the South Asian population prefers to communicate in their native language. For those individuals, speaking English can be a significant challenge. The recent shift towards online digital appointment booking systems has further distanced them from primary care access. A study involving 52 Bengali speakers in the UK demonstrated that nearly half of the participants faced difficulties in booking GP appointments through English digital platforms, such as eConsult. The various digital input methods and intricate typing involved in Bengali digital keyboards also make them unwieldy and demanding to use.
Lack of race-specific medical knowledge is another factor that contributes to healthcare inequality by delaying accurate diagnosis, optimal treatment, and preventive measures. For example, South Asians are at a higher risk of developing type 2 diabetes, and cardiovascular diseases, due to genetic and lifestyle factors. The occurrence of diseases resulting from bacterial infections, such as peptic ulcers and tuberculosis, demonstrates a markedly increased prevalence in patients of South Asian ethnic backgrounds [ Anderson S R, BMJ Thorax, 2007].
AI-assisted digital appointment booking, clinical triaging and patient management tools have gained popularity in recent years and have the potential to transform the healthcare industry. Nearly 300 GPs in England are testing the Klinik online triaging platform in order to ease the pressure on primary care. However, due to their inherent bias towards European patient data and languages, available AI-driven triaging systems fall short of adequately addressing racial disparities. If rolled out nationwide without addressing these Biases they will further perpetuate health inequalities. Healthcare authorities need to take a closer look at available AI-driven systems, and their ability to accommodate communities that have been historically deprived of healthcare.
To ensure AI-driven automation can deliver a truly inclusive healthcare system fit for the future, it is essential to increase diversity in data. Patients from different ethnic minority groups need to be involved throughout the development, testing and deployment of these systems. This can be achieved by establishing diversity and ethical standards in data collection and training AI models.

In conclusion, the under-representation of ethnic minority data in AI models is a crucial issue that can perpetuate discrimination and bias pushing these marginalised communities further away from healthcare. It's vital that AI technologies are developed with a commitment to diversity and inclusivity, ensuring that they reflect the full range of human experiences and perspectives. By addressing these biases, we can ensure that AI technologies can be used to benefit all members of society, regardless of their race or ethnicity.


5 Comments
Connor Gibson
Aenean eu leo quam. Pellentesque ornare sem lacinia quam venenatis vestibulum. Duis mollis, est non commodo luctus, nisi erat porttitor ligula, eget lacinia odio sem nec elit. Sed posuere consectetur est at lobortis integer posuere erat ante.
Nikolas Brooten
Quisque tristique tincidunt metus non aliquam. Quisque ac risus sit amet quam sollicitudin vestibulum vitae malesuada libero. Mauris magna elit, suscipit non ornare et, blandit a tellus. Pellentesque dignissim ornare faucibus mollis.
Pearce Frye
Cras mattis consectetur purus sit amet fermentum. Integer posuere erat a ante venenatis dapibus posuere velit aliquet. Etiam porta sem malesuada magna mollis.
Nikolas Brooten
Nullam id dolor id nibh ultricies vehicula ut id. Cras mattis consectetur purus sit amet fermentum. Aenean eu leo quam. Pellentesque ornare sem lacinia aenean bibendum nulla consectetur.
Lou Bloxham
Sed posuere consectetur est at lobortis. Vestibulum id ligula porta felis euismod semper. Cum sociis natoque penatibus et magnis dis parturient montes, nascetur ridiculus mus.