Breast cancer is the leading cause of death in women all over the world. In 2015, around 2.4 million women were diagnosed with breast cancer, with 523 000 dying[1]. Because breast cancer is more treatable when found early [2], many nations have implemented screening programs. To reduce breast cancer-related morbidity and mortality, one or two radiologists review a woman's mammograms for evidence of pre-symptomatic malignancy. Although mammography has proven to be an effective technique for the early identification of breast cancer and has considerably reduced mortality, the X-ray imaging method has limits, particularly for patients with dense breast tissue.
Challenges Currently Faced
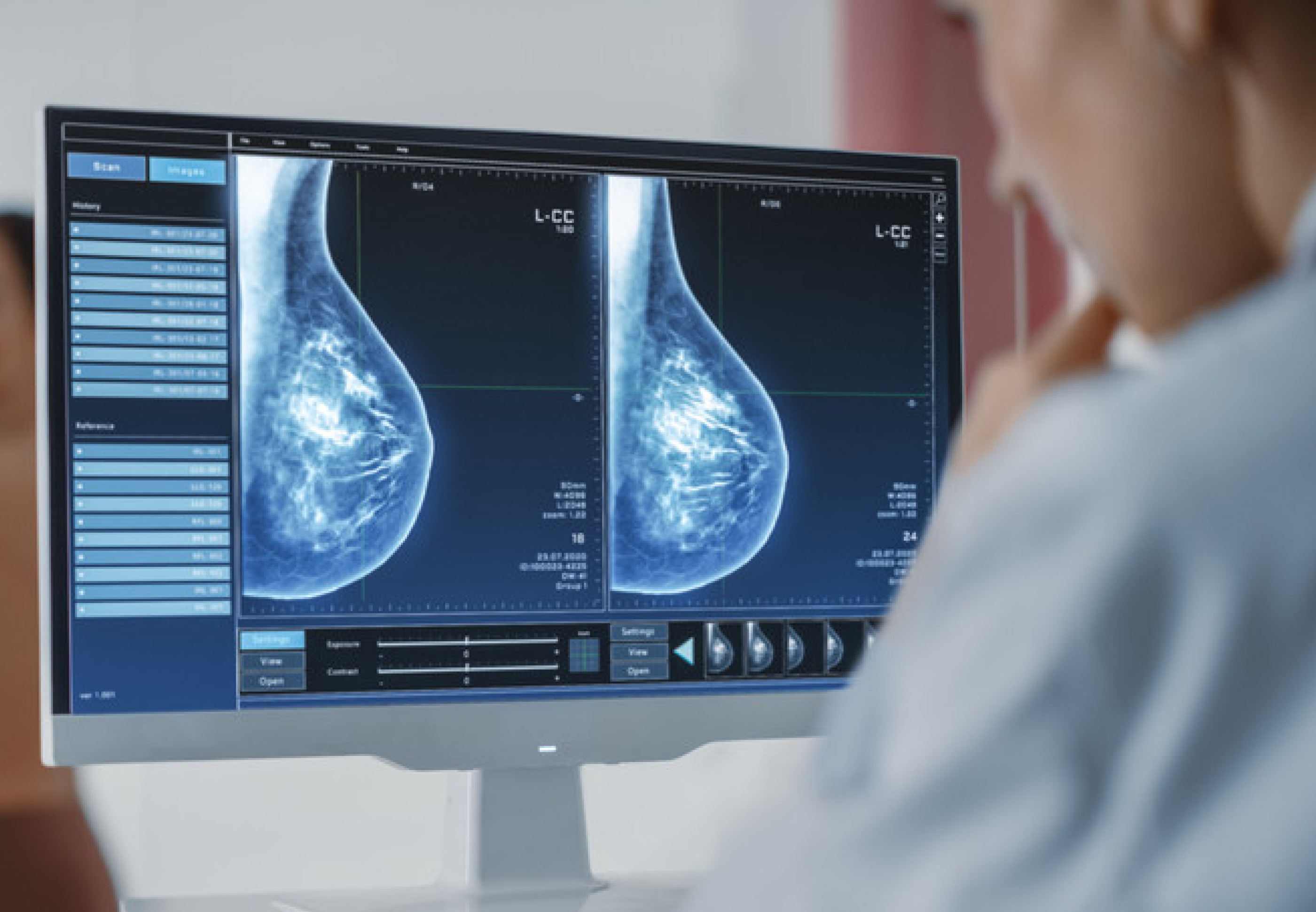
Mammography has helped reduce breast cancer-related fatalities by detecting the disease early when it is still treatable. It is, however, less responsive in women with dense breast tissue than in those with fatty breast tissue.
Furthermore, women with exceptionally dense breasts are three to six times more likely than women with virtually only fatty breasts, and two times more likely than the ordinary woman, to get breast cancer. Overdiagnosis and overtreatment of cancers that would not have become symptomatic within the woman's lifespan have been linked to such screening. There is disagreement on the level of overdiagnosis, which ranges from 1% to 54% of cancers diagnosed by screening, as well as the balance of advantages and harms of screening[2]. The range of diseases found during screening is extensive.
The spectrums of disease found at screening have an effect on the outcome. Discovery of low-grade ductal carcinoma in situ, for example, is more likely to result in overdiagnosis[3] [4], but detection of grade 3 cancer is more likely to result in fewer deaths. [5] During screening, cancer is diagnosed in 0.6 per cent to 0.8 per cent of women. [6] [7] Between 15% and 35% of malignancies are missed by breast screening programs, either due to human error or because the tumour is not apparent or detectable to the radiologist. Interval cancers are an indication of some of these overlooked malignancies. [8]
Another difficulty for radiologists is that, while mammograms produce high-resolution pictures, most asymptomatic cancer lesions are small, sparsely dispersed, and may only show minor changes in tissue patterns.
AI Technology
Artificial intelligence (AI) has the potential to improve both interpretative and noninterpretive tasks in breast imaging. AI-based screening triage may aid in the identification of normal examinations, and AI-based computer-aided detection (AI-CAD) may improve cancer diagnosis while reducing false positives.
Artificial Intelligence in mammography has exploded in popularity over the last few years. AI in mammography is a highly sought-after medtech innovation that has been featured in the news, presented at major radiology conferences and tradeshows, and even has its own scholarly journals.
Why is AI so popular in mammography?
The answer lies in the considerable value that this technology adds to patient diagnosis and care. Here are three advantages of AI in mammography, ranging from enhanced diagnostic confidence to increased efficiency.
Artificial intelligence boosts productivity
Mammography examinations on healthy women are scrutinized by radiologists for a long period (only 5 screening mammograms out of 1,000 contain cancers). AI-based algorithms allow breast imagers to move faster through cancer-free cases and pay greater attention to images with questionable discoveries by detecting and classifying abnormalities on mammograms, or by flagging their absence. In the end, we can expect more on-time mammography reading sessions are needed.
Burnout is reduced thanks to AI
Radiologists are constantly under pressure to read a big volume of images in a short amount of time, and the cost of an error is too high to make mistakes. The same can be said about the possibility of malpractice litigation. Stress levels are at an all-time high.
Even the best breast experts can have peace of mind with the help of an AI-powered tool. It indicates even if one feature is missing on an X-ray, letting the radiologist cross-check their judgment. Whereas radiologists’ performance tends to decrease once seventy or eighty minutes of reading, AI ever gets tired and has consistent performance. Through the utilization of AI in a diagnostic procedure, radiologists will feel assured and less anxious throughout their shifts.
Earlier Detection by AI
Sometimes to detect cancer, radiologists go back to analyzing prior scans only to discover that the abnormality was already present on the patient’s mammogram several years ago, though hardly visible. By using artificial intelligence in mammograms, cancer detection up to 2 years earlier is possible compared to human experts. Earlier detection means earlier treatment and a higher likelihood of survival.
On-going Research
"Specialists at NYU Langone's Perlmutter Cancer Center have reported that their artificial intelligence system has an accuracy rate of about 90 per cent, compared to an overall average of 80 percent by radiologistsArtificial intelligence can be a really good assistant because it helps read images faster, and our initial results found it was more accurate than radiologists,”
Since 2017, Dr. Moy has partnered with Krzysztof J. Geras, PhD, assistant professor in the Department of Radiology at NYU Grossman School of Medicine and a computer scientist affiliated with the NYU Center for Data Science, to develop artificially intelligent computer code that can “read” a mammogram and accurately predict the likelihood of breast cancer.
To train their system to differentiate between normal and suspicious tissue, the researchers fed it more than 2 million images drawn from mammograms performed at NYU Langone Health.
“Like facial recognition software, our computers can examine—in a split second—features that are otherwise imperceptible,”
“Notably, when radiologists used this tool as a second reader, their performance improved, So we want to reach that sweet spot where we use both.”
Conclusion
The Stand-alone Artificial Intelligence model might not be here yet. However, together with human radiologists and AI tools, we can definitely see a much greater success rate when it comes to analyzing mammography and ultimately saving lives.
References
- Fitzmaurice C, Allen C, Barber RM, et al., Global Burden of Disease Cancer Collaboration. Global, Regional, and National Cancer Incidence, Mortality, Years of Life Lost, Years Lived With Disability, and Disability-Adjusted Life-years for 32 Cancer Groups, 1990 to 2015: A Systematic Analysis for the Global Burden of Disease Study. JAMA Oncol2017;3:524-48. doi:10.1001/jamaoncol.2016.5688. Pmid:27918777
- Youlden DR, Cramb SM, Dunn NA, Muller JM, Pyke CM, Baade PD. The descriptive epidemiology of female breast cancer: an international comparison of screening, incidence, survival and mortality. Cancer Epidemiol2012;36:237-48. doi:10.1016/j.canep.2012.02.007. Pmid:22459198
- van Luijt PA, Heijnsdijk EA, Fracheboud J, et al. The distribution of ductal carcinoma in situ (DCIS) grade in 4232 women and its impact on overdiagnosis in breast cancer screening. Breast Cancer Res2016;18:47. doi:10.1186/s13058-016-0705-5. pmid:27160733
- Yen MF, Tabár L, Vitak B, Smith RA, Chen HH, Duffy SW. Quantifying the potential problem of overdiagnosis of ductal carcinoma in situ in breast cancer screening. Eur J Cancer2003;39:1746-54. doi:10.1016/S0959-8049(03)00260-0. pmid:12888370
- Tabar L, Chen TH, Yen AM, et al. Effect of Mammography Screening on Mortality by Histological Grade. Cancer Epidemiol Biomarkers Prev2018;27:154-7. doi:10.1158/1055-9965.EPI-17-0487. pmid:29150482
- Baines CJ, Miller AB, Wall C, et al. Sensitivity and specificity of first screen mammography in the Canadian National Breast Screening Study: a preliminary report from five centers. Radiology1986;160:295-8. doi:10.1148/radiology.160.2.3523590. pmid:3523590
- Houssami N, Macaskill P, Bernardi D, et al Breast screening using 2D-mammography or integrating digital breast tomosynthesis (3D-mammography) for single-reading or double-reading--evidence to guide future screening strategies. Eur J Cancer2014;50:1799-807. doi:10.1016/j.ejca.2014.03.017. Pmid:24746887
- Houssami N,Hunter K. The epidemiology, radiology and biological characteristics of interval breast cancers in population mammography screening. NPJ Breast Cancer2017;3:12. doi:10.1038/s41523-017-0014-x. Pmid:28649652
- https://nyulangone.org/news/can-artificial-intelligence-perfect-mammography


5 Comments
Connor Gibson
Aenean eu leo quam. Pellentesque ornare sem lacinia quam venenatis vestibulum. Duis mollis, est non commodo luctus, nisi erat porttitor ligula, eget lacinia odio sem nec elit. Sed posuere consectetur est at lobortis integer posuere erat ante.
Nikolas Brooten
Quisque tristique tincidunt metus non aliquam. Quisque ac risus sit amet quam sollicitudin vestibulum vitae malesuada libero. Mauris magna elit, suscipit non ornare et, blandit a tellus. Pellentesque dignissim ornare faucibus mollis.
Pearce Frye
Cras mattis consectetur purus sit amet fermentum. Integer posuere erat a ante venenatis dapibus posuere velit aliquet. Etiam porta sem malesuada magna mollis.
Nikolas Brooten
Nullam id dolor id nibh ultricies vehicula ut id. Cras mattis consectetur purus sit amet fermentum. Aenean eu leo quam. Pellentesque ornare sem lacinia aenean bibendum nulla consectetur.
Lou Bloxham
Sed posuere consectetur est at lobortis. Vestibulum id ligula porta felis euismod semper. Cum sociis natoque penatibus et magnis dis parturient montes, nascetur ridiculus mus.